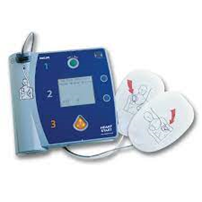
First approved for public use in the 1970s, an Automated External Defibrillator (AED) is a computerized medical device that can be used to reverse some lethal heart rhythms during cardiac arrest. While it does not take the place of high-quality CPR, it is the only definitive treatment modality available outside of a hospital or advanced life support (paramedic-level staffed) ambulance.
On January 1, 2012, the New York State Dental AED Law (S2923) went into effect. Every dentist in New York State, regardless of practice size, is required to have and properly maintain an AED. This means that the device must be approved by the FDA and that all consumable items (electrode pads and batteries) must be maintained in accordance with manufacturer guidelines. Only items within current expiry are allowed to remain in service. In addition, the device must be capable of recording data during a resuscitation attempt, and that data MUST be forwarded to the local Medical Control authority within 72 hours.
Non-compliance with any part of this law is subject to disciplinary action held against your dental license by the New York State Education Department Office of the Professions.
As an added layer of protection, every AED manufacturer offers both a warranty for their products, and a statement of indemnification—a promise to stand behind the user when a properly maintained unit becomes the subject of civil litigation. If you purchased your AED prior to 2015, the warranty and indemnity have likely expired.
In the 40+ years since they were first developed, and 11 years since this law first went into effect, the technology available has advanced. While the original AED technology uses a one-size-fits all approach to defibrillation, newer technologies utilize data from the patient (i.e., body mass index, amplitude of a fibrillation wave) to determine an appropriate shock dose. Newer technology will increase subsequent shock doses as the heart becomes increasingly refractory to defibrillation resulting from hypoxia and consequent fermentation. In support of the current push toward high-quality CPR, newer AEDs may also be equipped with technology that can measure the depth and rate of chest compressions administered by the resuscitation team and will provide real-time feedback to improve and maintain high-quality CPR, further reducing the effects of hypoxia and fermentation.
Some newer units are also able to recognize and properly treat Supraventricular Tachycardia (SVT) through cardioversion, something that cannot be accomplished with older technology. Delivery of shocks in some newer units may also be fully automatic, reducing the need to depend on a human to push the shock button in a potentially high-stress moment.
Units That MUST Be Replaced IMMEDIATELY
The following AEDs have been discontinued, are no longer supported by the manufacturer, do not have FDA-approved electrode pads and batteries available, and no longer carry ANY manufacturer warranty or indemnity. In addition, the software in the units may NOT be compliant with the same 2010 Emergency Cardiac Care (ECC) Guidelines taught in modern-day CPR classes, and so will not behave as expected during a resuscitation effort. These units cannot reliably affect a rescue, leaving you essentially without any AED available for your office.
Units That Should Be Replaced VERY SOON
ANY unit that is outside of its warranty / indemnity period should be replaced. Some AEDs may have some trade-in value left, depending on make, model and date of manufacture.
Philips continues to experience quality control issues with their monitor / defibrillator products and is currently operating under consent decree by the FDA. This forced Philips to suspend some operations from November 2017 until April 24, 2020. In the summer of 2022, Philips announced additional quality control problems with their electrode pads in which the glue may discolor or fold upon itself. According to their letter, there are no plans to fix the problem—instead Philips suggests unfolding the glue on the pads and ignoring discoloration during a rescue.
Philips purchased the Onsite and FRx designs in 2000 when it acquired Agilent healthcare group. Nearly twenty-five years later, the same rudimentary technology exists within both models.
Replacement AED Recommendations
Although we have relationships with every AED manufacturer, I have narrowed down three recommendations for your consideration, from most to least expensive. My recommendations are based upon technological advancement, quality, cost, and product availability.
Cardiac Science Powerheart G5
The technology in this unit is truly amazing. In addition to a seven-year warranty/indemnity, technical and customer support for the unit, availability of manufacturer and FDA-approved electrode pads and batteries, and compliance with the New York State Dental AED Law (S2923), every technological advancement available is in this unit. In addition, this is the only AED manufacturer on the market that offers a power gauge for users to easily determine the battery life that remains. Unfortunately, with better technology comes increased costs to replace the battery and pads.
Cardiac Science Powerheart G3
This unit is no longer in production, as it has been replaced by the upgraded Cardiac Science G5. However, all of the technology of the G5 is still inside this unit, except the rate and depth of compressions cannot be measured and subsequent feedback is not provided to rescuers. This unit is being offered as a recertified AED, with a four-year warranty. This means that the unit has been rigorously tested by a manufacturer-certified technician. The unit comes with a new battery and pads and replacements are available for the foreseeable future. The replacement battery is a bit pricy, but the warranty will expire before a new battery is needed.
Defibtech Lifeline
This AED utilizes standard technology that has not evolved much from the original 40-year-old design. However, a new unit does offer the benefits of a warranty / indemnity for the next eight years, technical and customer support for the unit, availability of manufacturer and FDA-approved electrode pads and batteries, and compliance with the New York State Dental AED Law (S2923).
This unit is available to deliver a shock both manually and fully automatically. Most standard-technology units do not have this feature.
AED Comparisons
| Prices Effective June 1, 2024 | Philips OnSite | Cardiac Science G5 | Cardiac Science G3 | Defibtech Lifeline |
| AED Type | New | New | Recertified | New |
| Warranty | 8 Years | 7 Years | 4 Years | 8 Years |
| Battery Life | 4 Years | 4 Years | 4 Years | 5 Years |
| Pads Life | 2 Years | 2 Years | 2 Years | 2 Years |
| Shock Delivery | 150J Semi Automatic | Customized, Escalating Semi or Fully Automatic | Customized, Escalating Semi or Fully Automatic | 150J Semi Automatic Available as fully automatic (+$110) |
| Waveforms Recognized | V-Fib V-Tach | V-Fib V-Tach SVT | V-Fib V-Tach SVT | V-Fib V-Tach |
| Estimated Cost To Own Over Warranty Period Current Retail Prices | $61 per year | $183 per year | $135 per year | $52 per year |
| Retail | $1,479 | $2,064 | $995 | $1,370 |
| Client Incentive* | -$150 | -$100 | -$150 | |
| NYS Tax Credit† | $500 | $500 | $500 | $500 |
| Total Cost (with all credits) | $979 | $1,414 | $395 | $720 |
| YOU PAY TODAY‡ | $1,479 | $1,914 | $895 | $1,220 |
Pediatric pads can be added to any of the AEDs above, for an additional $120 per set. The cost of these pads is added to the final “out of pocket” cost and is not subject to member incentive discounts. Pediatric pads are not included in the estimated cost to own.
*Client incentives are provided exclusively to members who agree to a maintenance agreement at NO ADDITIONAL COST. This agreement will allow Have Dummy Will Travel, Inc. to send replacement AED electrode pads within one month prior to expiry and battery replacement upon device warning with the promise of invoice payment on NET 30 terms. The agreement will be in force as long as the AED is owned by the client.
†Filing for the NYS Tax credit is the responsibility of the member. Tax forms containing pertinent information will be provided upon completion of the final transaction.
‡ This offer requires payment via cash, check, money order, Zelle or Venmo only. An additional 3.99% service fee will be added to any credit card payments. Philips brand products requires a credit card only for purchase but is not subject to any additional service fee.